AI-Powered Appointment Scheduling for UK Physiotherapy Practices: The Complete Guide to Reducing Admin & No-Shows
The Reality of Revenue Leakage
You’re losing money every time your phone rings and no one picks up. Sounds dramatic, but let’s put numbers to it: if your average physiotherapy session is worth £65 and you miss three potential bookings a week because Karen was on lunch and the answering machine kicked in, that’s £10,140 annually. Just gone. And honestly, three missed calls feels conservative—most practices I’ve looked at are closer to eight or ten.

But here’s the bit that really stings. It’s not just missed calls. It’s the “phone tag” afterwards. Patient calls at 11:34 AM, you’re with someone. You ring back at 2:17 PM, they’re at work. They text “can you call after 6?” You’re gone by then. This timing tennis eats up receptionist hours and, more importantly, patient enthusiasm cools with every day that passes. By the time you finally connect, they’ve either booked elsewhere or decided to “see how it goes” (spoiler: they won’t book).
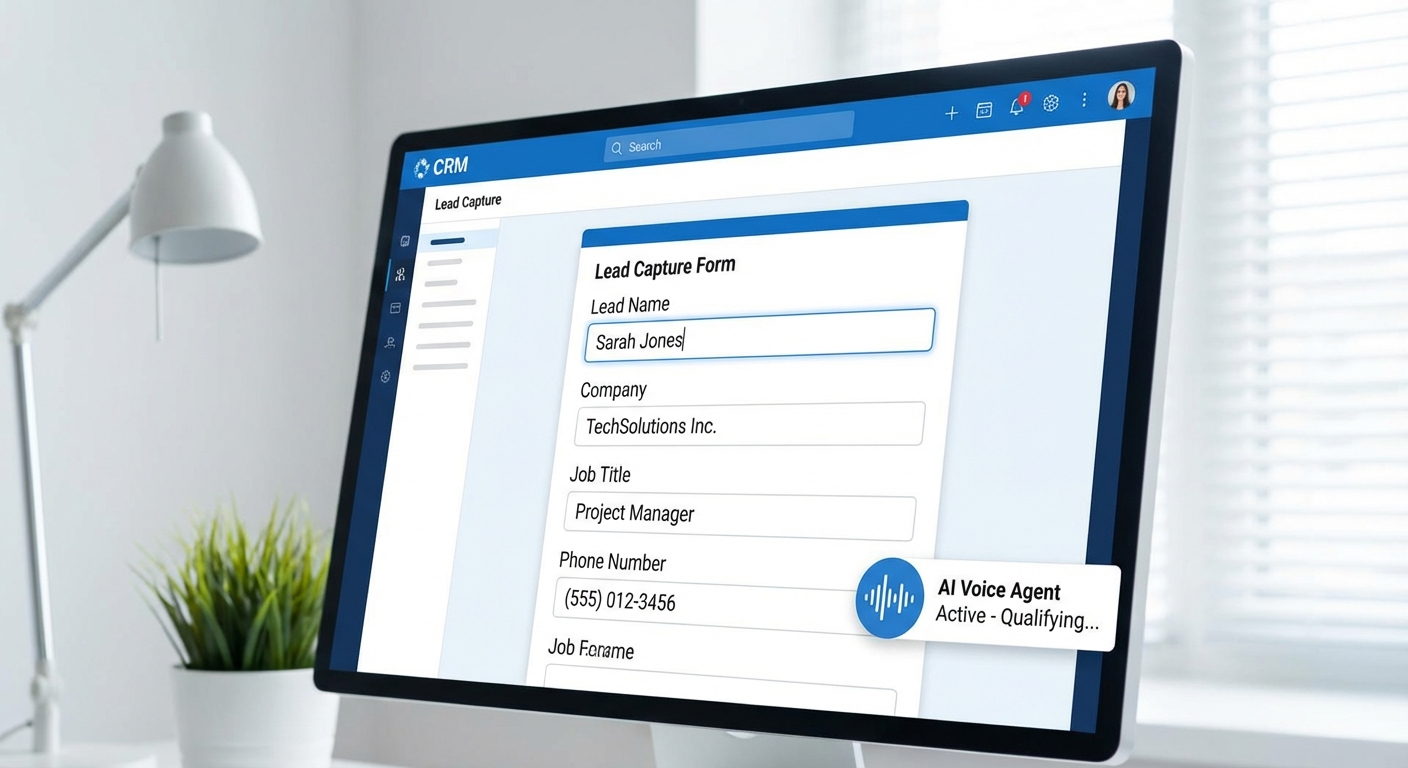
What I want you to think about is something I’m calling the “Hybrid Reception” model. Not replacing your front desk staff—let me be clear on that—but augmenting them with an AI layer that operates round the clock. Think of it as having a digital receptionist who never sleeps, never takes a lunch break, and can handle five conversations simultaneously at 2 AM when someone’s lower back has finally convinced them to stop scrolling Reddit and actually book help.
This guide focuses specifically on UK practices because the integration landscape here is unique. You’re likely using Cliniko, TM3, or maybe WriteUpp. You need to think about GDPR differently than our US counterparts. And frankly, if the NHS—with all its bureaucratic machinery—is successfully deploying AI scheduling (which they are, we’ll get to that), then private practices should be able to move faster and capture the commercial upside.
The Admin Crisis in UK Physiotherapy: Why Traditional Booking is Failing

The Bottleneck of Manual Intake
Most physiotherapy websites still have a “Contact Us” form that might as well say “we’ll get back to you… eventually.” Patient fills it out. Form lands in someone’s inbox. That someone checks email twice a day if you’re lucky. Then someone has to ring back during business hours to actually complete the booking.
Meanwhile, your competitor has a “Book Now” button that works at midnight.
A 9-to-5 reception desk made sense in 1987. It makes zero sense now when patient pain and booking intent don’t respect office hours. I’ve seen analytics from practices that added 24/7 booking—23% of their appointments were initiated outside traditional business hours. Nearly a quarter. Now, I’d want to know more about what “initiated” means here (did they complete the booking or just start it?), but even half that number represents patients who would have either called a competitor the next morning or talked themselves out of treatment entirely.
And then there’s staff burnout. Repetitive admin tasks—rescheduling the same patient three times because they can’t quite commit to a Tuesday—drain morale in ways that don’t show up on an HR report until someone hands in their notice. Your reception team didn’t train to read the same script forty times a day. They’re capable of so much more, but transactional volume buries them.
Lessons from the NHS: Evidence that AI Scheduling Works
Right, so here’s where it gets interesting. NHS launched the UK’s first AI-powered physiotherapy clinic through a company called Flok Health in 2024. The NHS. Not exactly known for rapid tech adoption.
Results? They more than halved back pain waiting lists. Achieved 98% success rate with digital triage. And get this—only 3% of patients needed referral to traditional pathways, meaning the AI correctly handled the vast majority of cases without human intervention in the scheduling and initial assessment phase. (I’m honestly surprised it’s only 3%, though I’d want to see what “correctly handled” actually means in their methodology.)
Think about what that means for a private practice. NHS has to navigate privacy regulations, clinical governance frameworks, and union negotiations. They still made it work because efficiency gains were undeniable. If they can deploy AI to reduce no-shows and admin burden in a bureaucratic environment, you—with direct control over your operations and a clear commercial incentive—can pivot faster.
Flok Health’s model used same-day digital appointments via app, which fundamentally changed patient behaviour. When people can book and be seen quickly, they show up. Waiting list reduction wasn’t just about seeing more patients; it was about capturing intent at the moment of maximum motivation.
2026 and Beyond: The Software Trend Forecast
PhysioCare PMS’s 2026 trends analysis shows something you need to pay attention to: intelligent scheduling bots are moving from luxury feature to standard expectation. We’re talking about systems that don’t just fill calendar slots—they predict cancellations before they happen based on patient behaviour patterns.
For instance, if a patient has cancelled their last two Friday afternoon appointments, the AI flags this and either avoids booking them on Friday afternoons or automatically sends an extra confirmation. Some systems are now analyzing factors like distance to clinic, weather conditions, and even local traffic patterns to assign a “show-up probability” to each booking.
This is physiotherapy practice management software evolving from passive databases (basically just fancy filing cabinets) to active operational tools that make decisions. Software becomes a team member, not just a record keeper.
I’m not entirely sure every practice needs the most sophisticated version of this right out the gate, but the trajectory is clear. Within eighteen months, patients will expect instant booking confirmation at whatever hour they decide to sort out their neck pain. Practices that can deliver that will eat lunch from those that can’t.
Defining the “Hybrid Reception” Model for Private Clinics


Beyond Simple “Book Now” Buttons
A standard online booking calendar is static. It shows available slots. Patient clicks one. Done. That’s helpful, sure, but it’s not intelligent.
AI-powered scheduling is dynamic. It understands context. When someone says “I need an emergency appointment for acute back pain that started yesterday and I can barely stand,” the AI doesn’t just find the next available slot three days from now. It recognizes urgency, checks if there’s a cancellation today, and might even suggest a longer initial assessment slot rather than the standard 30-minute follow-up.
AI acts as both digital triage nurse and receptionist. It’s asking qualifying questions: “Is this a new injury or ongoing condition?” “Have you had physiotherapy before?” “Are you using private insurance or self-pay?” These answers determine which practitioner is most appropriate and how much time to allocate.
Genuinely different from a dropdown menu. System is making clinical and operational judgments, not just calendar management.
The 24/7 Patient Intake System
Here’s the mechanism that actually shifts the model. An automated clinic reception tool—let’s say a chatbot embedded on your website—captures patient data whenever someone visits. Could be Tuesday at 10 AM or Saturday at 1:43 AM.
Workflow looks like this: Patient interacts with AI agent through conversational interface (not filling out a rigid form). AI asks dynamic questions based on previous answers. “You mentioned shoulder pain—does it hurt when you lift your arm overhead?” Based on responses, AI pre-qualifies the patient. Are they self-pay or do they have Bupa/AXA coverage? Do they need a sports injury specialist or someone focused on post-surgical rehab?
Then AI books the slot directly into your practice management system, with the clinician who has both availability and relevant specialization.
Value here is capturing the “midnight scrollers.” People who experience pain, can’t sleep, start googling solutions, find your website, and are in a mindset to make decisions immediately. If your only option is “call us tomorrow,” you’ve lost them. If they can book and receive confirmation in three minutes at 1 AM, you’ve gained a patient.
Human-in-the-Loop Architecture
Let me be very clear about something because I’ve seen this fear derail conversations: this is not about making reception staff redundant.
It’s about role evolution. Your team stops spending 60% of their day answering “what time are you open?” and “do you take Bupa?” and “can I reschedule my Thursday?” Those questions are transactional. They don’t require human judgment or empathy. They’re also mind-numbing.
Role shift looks like this: AI handles transactional volume—bookings, basic questions, straightforward reschedules. Human staff handle relational value—greeting patients warmly when they arrive, managing complex billing disputes, having the sensitive conversation when someone needs to discuss payment plans, noticing when a regular patient seems off and checking in with them.
Your receptionist becomes more of a patient experience coordinator. Which, honestly, is a much better use of a human brain and much more fulfilling work.
Efficiency mathematics work because AI can handle five conversations simultaneously. Your human staff can’t. But your human staff can read body language, pick up on emotional distress, and exercise judgment in ambiguous situations. AI can’t do that. Well, not reliably—don’t believe vendor promises about emotion recognition.
Hybrid architecture means patients get fast, accurate responses for routine stuff, and meaningful human interaction when it matters.
Mechanisms for Reducing Patient No-Shows via AI

Predictive Analytics and Risk Scoring
You can’t fix what you can’t measure, and most practices have no idea which bookings are at highest risk of no-show until the patient simply doesn’t appear.
AI changes this by analyzing patient history to assign a probability score. System looks at: previous cancellation patterns (did they cancel last minute before?), distance to clinic (patients traveling more than 30 minutes are statistically less likely to show), booking lead time (appointments made more than two weeks out have higher no-show rates), and even time of day (early Monday morning appointments see more cancellations than midweek slots).
Based on these factors, AI flags high-risk bookings. A simple dashboard shows your reception team which Thursday appointments are most likely to flake. Now you can take action—make a personal confirmation call, send an extra reminder, or even overbook slightly in that slot knowing there’s a 40% chance the patient won’t show.
Actionable output is what matters here. Predictive data without action is just anxiety-inducing trivia. But when the system tells you “this 8 AM Friday booking is 73% likely to cancel,” and you ring that patient Wednesday afternoon to confirm, you’ve either reinforced their commitment or freed up the slot in time to offer it to someone else.
I’ve seen practices reduce no-shows by 30-40% just from implementing risk scoring and acting on the flags. That’s not magic. That’s just knowing where to focus limited human attention.
Smart Reminders vs. Static SMS
Most practices send the same text reminder 24 hours before every appointment. “You have an appointment tomorrow at 3 PM.” Patient receives it, acknowledges it mentally, forgets about it.
Smart reminders use dynamic timing based on patient engagement patterns. If someone consistently reads messages in the evening, AI sends their reminder at 7 PM rather than 2 PM when it might get buried. If someone prefers WhatsApp over SMS (you can tell from response rates), system uses that channel.
More importantly, these are two-way conversations. Patient receives reminder. They can reply “need to reschedule” and AI immediately offers alternative slots via text. No need to call the clinic, navigate phone menus, or wait on hold. Whole rescheduling transaction happens in three text messages over ninety seconds.
But here’s the mechanism that really drives utilization: automated waitlist management. Patient cancels at the last minute. AI instantly identifies three patients on a digital waitlist who live nearby and have indicated availability on short notice. It sends them an offer: “Slot available today at 3 PM—interested?” First person to respond gets it.
This can push your utilization rate toward 100%, which fundamentally changes practice economics. Every empty slot is revenue you can never recover. AI doesn’t eliminate cancellations (people have genuine emergencies), but it eliminates revenue loss from cancellations.
Pre-Appointment Engagement
Here’s a psychological trick that works: the moment someone books, send them something valuable. Could be a video explaining what to expect in their first appointment. Could be a pre-hab exercise relevant to their condition. Could be a digital intake form that has them describe their history in detail.
Content itself matters less than the commitment mechanism. When a patient spends five minutes filling out a detailed history form or watching your welcome video, they’re psychologically invested. They’ve already begun the treatment relationship. They’re much less likely to casually cancel.
NHS AI clinic expansion across eleven regions (reported by Building Better Healthcare) showed this principle at scale. Digital engagement before appointments improved patient adherence significantly. When patients interacted with AI system multiple times before their appointment—booking, confirming, completing intake—they developed a sense of momentum toward treatment.
You’re essentially using the psychological principle of consistency. Small commitments (filling out a form) make people more likely to follow through on larger commitments (actually showing up). And AI automates delivery of these engagement moments immediately after booking, when enthusiasm is highest.
Technical Integration: Connecting AI with UK Practice Management Software

The API Ecosystem (Cliniko, TM3, WriteUpp)
Where the rubber meets the road technically, and I won’t pretend it’s always smooth.
Core requirement: your AI scheduling tool must be able to read and write directly to your existing practice management system via API (Application Programming Interface, but you probably already knew that). Without this integration, you’re just creating more admin work—someone has to manually transfer bookings from AI system into your PMS, which defeats the entire purpose.
Cliniko and TM3 both offer reasonably robust APIs. AI system needs to see real-time availability for specific practitioners. Not just “the clinic is open Tuesday at 2 PM” but “Sarah, your sports injury specialist, has a 45-minute slot at 2 PM, but James only has 30 minutes at 2:15 PM.”
Conflict resolution is critical. Here’s the scenario that causes problems: your receptionist is on the phone with a patient, checking availability. Simultaneously, someone on your website is interacting with AI. They’re both looking at the same 3 PM slot. Receptionist books it verbally. Two seconds later, AI books it for the website patient. Congratulations, you’ve double-booked.
Proper integration handles this through real-time locks. Moment the receptionist clicks into that slot, it’s temporarily locked. AI can’t book it. Or vice versa. This requires PMS and AI system to communicate constantly, not just sync once every five minutes.
Some AI vendors claim integration but actually just scrape your booking page like a human would. This causes exactly the conflicts I just described. Ask vendors explicitly: “Is this a bidirectional API integration or screen scraping?”
Data Synchronization and Note Taking
Really sophisticated systems do automated intake that populates your clinical records before patient arrives.
AI collects subjective history through conversation: “When did the pain start?” “Is it worse in the morning or evening?” “Have you had imaging done?” “Previous injuries to this area?” Basic SOAP note elements—Subjective, Objective, Assessment, Plan—at least the subjective portion.
Information flows directly into patient file in your PMS. When your physiotherapist opens the chart thirty seconds before appointment, they already have two paragraphs of history. That saves 5-10 minutes per session that would normally be spent on intake questions.
Those minutes compound. If you see six patients a day and save eight minutes per patient, that’s 48 minutes. Nearly a full extra appointment slot you can offer. Across a five-day week, that’s four hours of recovered clinical time that can be monetized or used to reduce working hours (probably the former if we’re being honest).
Technical challenge is ensuring AI captures information in the format your physiotherapists actually want. If your team uses a specific subjective history template, AI output needs to match that structure. Otherwise you’ve just moved admin work from pre-appointment to mid-appointment reformatting.
Technical Requirements for Setup
Cloud-based systems are non-negotiable at this point. On-premise servers made sense when data security meant physical control. Post-GDPR, cloud providers with proper security certifications are often more secure than a practice’s local server gathering dust in a closet.
Performance factor: real-time syncing is essential. If there’s a five-minute delay between someone booking online and that appointment appearing in your PMS, you will have conflicts and frustrated patients. Latency has to be measured in seconds, not minutes.
So you need reliable internet connectivity. If your clinic’s WiFi drops out twice a day, you’re going to have problems with AI scheduling that depends on constant cloud communication. Sort out your infrastructure before adding sophisticated software on top of it.
Most cloud-based AI systems work via browser—no installation required. Your team logs in from any device. But this also means if someone loses their laptop, you need proper two-factor authentication and immediate access revocation capability, which brings us to the next section.
Regulatory Compliance: Navigating GDPR and CQC in an AI World

Data Sovereignty and UK GDPR
First question to ask any AI vendor: where is patient data hosted?
Post-Brexit, UK GDPR requires either UK hosting or EU hosting with adequacy agreements. If your vendor stores data in US servers, you’re in murky legal territory unless they have Standard Contractual Clauses in place. Most UK practices don’t have the legal budget to navigate this complexity, so the simple rule: insist on UK or EU data hosting.
Consent flow matters. When a patient first interacts with your AI booking system, they need clear information about how their data will be processed. Can’t be buried in a 4,000-word privacy policy. It needs to be explicit at point of interaction: “We use AI to manage bookings. Your information is stored securely and used only for appointment scheduling and clinical care. Full privacy policy here.”
GDPR’s “right to erasure” gets complicated with AI systems. If a patient requests deletion of their data, does that include anonymous training data that improved the AI model? Most regulators say yes to direct identifiable data, no to fully anonymized aggregate data. Make sure your vendor has a clear data deletion process that you can action quickly.
I’m frankly surprised how many AI vendors still give vague answers about data location. If they can’t tell you within ten seconds which specific data centers host UK patient information, keep looking.
Clinical Safety and CQC Standards
Care Quality Commission has approved AI-powered clinics (like Flok Health’s NHS example), which sets a safety benchmark. But approval doesn’t mean absence of risk.
Critical safety feature: red flag triage. Your AI must recognize emergency symptoms and direct patients appropriately. If someone describes potential Cauda Equina Syndrome symptoms—saddle anesthesia, bladder dysfunction, bilateral leg weakness—AI should not book them for a physio appointment next Tuesday. It should tell them to go to A&E immediately.
This requires clinical content design by actual clinicians, not just software developers optimizing for booking conversions. AI logic needs to prioritize safety over efficiency. Ask vendors: “Who designed your clinical triage algorithms? Are they reviewed by UK-qualified physiotherapists or medical professionals?”
CQC inspections will eventually catch up to AI adoption. When an inspector asks “how do you ensure clinical safety in your digital intake process,” you need documentation. That means audit trails showing AI’s decision-making, evidence of clinical oversight in system design, and protocols for human review of complex cases.
Vendor Due Diligence Checklist
Before signing contracts, work through this systematically.
Security Protocols
Encryption standards matter. Minimum should be AES-256 encryption for data at rest and TLS 1.2 or higher for data in transit. If a vendor can’t confirm this, walk away.
Two-factor authentication (2FA) for anyone accessing admin system is essential. Someone’s receptionist logs in from home on their personal laptop—if that laptop gets compromised, you need 2FA as a second line of defense.
Regular penetration testing. Ask when system was last pen-tested and by whom. “We take security seriously” is not an answer. “We commissioned a pen test by [specific firm] in November 2024, here’s the executive summary” is an answer.
Transparency
UK consumer protection law requires clear labeling when someone is interacting with an AI, not a human. Your booking interface needs to indicate this upfront. “This is an automated system” or “You’re chatting with our AI assistant.”
Some patients prefer human interaction for various reasons—accessibility needs, complexity of their case, or just personal preference. AI system must offer an easy escalation path: “Speak to a human instead” button that actually connects them to your reception team during business hours.
(Okay, you definitely already know this part, but it’s worth stating: transparency builds trust, which reduces complaints and regulatory scrutiny. It’s not just compliance box-ticking.)
Commercial Analysis: ROI and Private Practice Growth

Calculating the Cost of Inefficiency
Most practice owners have a rough sense they’re losing money to admin inefficiency. But rough sense doesn’t motivate investment. Specific numbers do.
Here’s the formula: (Average Appointment Value × Missed Appointments per Month) + (Reception Staff Hourly Rate × Admin Hours Saved per Month) – (AI Tool Subscription Cost).
Let me make this concrete with realistic numbers. Your average appointment is £62. You estimate you miss five bookings monthly due to phone tag, full voicemail, or delayed responses. That’s £310 lost revenue. Your receptionist earns £13/hour and spends roughly 25 hours monthly on rescheduling calls and back-and-forth booking confirmations. That’s £325 in labor costs. So your monthly inefficiency cost is £635.
Most AI scheduling tools for small practices run £200-400 monthly. Let’s say £300. Your net monthly gain is £335, or just over £4,000 annually. But this is conservative because it doesn’t account for bookings you capture at 11 PM on a Saturday that you’d never get otherwise.
Revenue recovery happens fast. Filling just two extra slots weekly at £62 each covers cost of most AI tools and then adds £6,448 annually in pure growth. Practices report 15-25% increases in bookings within three months of deploying 24/7 scheduling because you’re no longer limited by reception hours.
Scalability for Multi-Site Clinics
If you operate multiple locations, economics get even more compelling.
Traditional model: each location needs reception coverage. Two locations mean two receptionists minimum. Three locations, three receptionists. Labor costs scale linearly with expansion.
AI model: centralized booking across all locations. One AI system manages appointments for your Harley Street clinic, your Birmingham satellite office, and your Manchester location. Patients book at any location based on availability and proximity. You need fewer reception staff overall because AI handles transactional volume across all sites.
Building Better Healthcare’s article on AI clinic expansion across eleven NHS regions demonstrates this scalability. A single AI platform managed appointments across geographically dispersed locations. Operational model is directly applicable to private practice chains looking to expand without proportionally increasing admin overhead.
I’ve seen a three-location MSK practice in the Midlands reduce from five reception staff to two after implementing centralized AI scheduling. People who left weren’t made redundant—they were reassigned to other roles as practice grew (one became a practice manager, actually). But the point stands: expansion didn’t require hiring more admin staff.
Patient Acquisition Cost (CAC)
Look, you’re probably spending money on Google Ads or Facebook campaigns to drive traffic to your website. Conversion rate from website visitor to booked appointment is your critical metric.
Traditional booking: visitor clicks “contact us,” fills form, waits for callback. Conversion rate might be 8-12% because enthusiasm leaks away during waiting period. Some never hear back because form went to spam. Some find another provider while waiting.
Instant AI booking: visitor finds available slot, books immediately, receives confirmation within sixty seconds. Conversion rate jumps to 25-35% because there’s no friction or delay between intent and action.
Marketing spend becomes more efficient. If you’re paying £8 per click and your conversion rate doubles, your cost per acquired patient halves. Same ad budget generating twice as many appointments. Or you can maintain same patient volume with half the ad spend and pocket the difference.
Every practice owner I know is obsessed with reducing patient acquisition cost. Removing booking friction is probably the highest-impact action you can take without touching your actual marketing campaigns.
Selecting the Right Tool: A Buyer’s Framework

Key Features to Look For
Natural Language Processing (NLP) quality varies wildly between systems. Test this during demos. Type “sore neck since this morning, probably slept wrong” and see how AI responds. Does it understand that’s a musculoskeletal issue requiring standard assessment? Or does it get confused and ask irrelevant questions?
AI should grasp colloquial descriptions. Real patients don’t say “I’m experiencing lateral epicondylitis.” They say “my elbow hurts when I lift stuff.” System needs to translate patient language into clinical categories that inform appropriate practitioner selection and time allocation.
Omnichannel support matters for reaching patients where they already are. Website widget is baseline. But can it also handle inquiries via Facebook Messenger? WhatsApp? SMS? Different demographics prefer different channels—younger patients might prefer Instagram DMs while older patients stick to phone calls (which AI can handle through voice recognition, though that’s still imperfect).
UK market understanding matters more than you’d think. System needs to recognize private insurance codes for Bupa, AXA, Aviva, WPA, Vitality. It should understand NHS referral pathways if you accept those. It needs to work with UK postcodes, not just zip codes. Some US-developed systems require painful customization to work properly in UK practices.
Also check: does system understand British English? I’ve seen AI tools trained primarily on American medical terminology that get confused by “physiotherapy” instead of “physical therapy” or stumble over UK-specific terms.
Implementation Roadmap
Don’t go from zero to full AI deployment overnight. That’s how things break and staff mutiny.
Phase 1 is shadow mode. AI monitors conversations and suggests responses, but doesn’t take action. Your reception team sees what AI would have said or booked. Training period lets everyone build confidence in system’s accuracy. Run this for 2-3 weeks.
Phase 2 is hybrid mode. AI handles out-of-hours inquiries only. During business hours, humans still manage booking. This gives you time to identify and fix problems when stakes are lower. No-one expects perfect service at 2 AM, so it’s a safer testing ground. Run this for 4-6 weeks.
Phase 3 is full deployment. AI handles all primary intake, during and after hours. Humans focus on complex cases, personal touch, and patient care. Even at this stage, maintain human escalation paths for patients who prefer it or have complicated situations AI flags for review.
Some practices never move to Phase 3, staying in permanent hybrid mode. That’s fine. Goal isn’t maximum automation; it’s optimal efficiency while maintaining quality of care and patient satisfaction.
Red Flags in AI Vendors
Lack of integration with major UK PMS providers is disqualifying. If they say “we’re working on Cliniko integration” but don’t have it live yet, pass. You’re not a beta tester unless they’re paying you to be one.
Vague answers about data storage location suggest they don’t take GDPR seriously or don’t understand UK requirements. If they say “we use AWS” but can’t specify which regional data centers, that’s not good enough.
Over-promising medical advice capabilities should trigger alarm bells. If a vendor claims their AI can provide clinical treatment recommendations or diagnose conditions, they’re either ignorant of regulatory boundaries or deliberately misleading you. AI can triage (sort by urgency), schedule, and collect history. It should not be diagnosing or advising treatment. That requires MHRA medical device approval and brings liability issues you don’t want.
Other concerning signs: no clear pricing structure (if they won’t tell you cost upfront, it’s probably expensive and they want to lock you in emotionally first), no trial period or demo access, pushy sales tactics that pressure immediate decisions, and lack of references from existing UK physiotherapy practices.
Ask for three referee contacts—actual UK clinics using system. Call them. Ask about implementation challenges, hidden costs, and whether they’d choose same vendor again.
Summary: The New Standard of Care
Hybrid Reception model delivers three core benefits: operational efficiency (your team does more meaningful work), regulatory compliance (when properly implemented), and revenue protection (capturing bookings that would otherwise leak away).
Anyway, this isn’t futurism. It’s already happening. NHS deployment proves viability at scale under stringent safety and governance requirements. Private practices have fewer constraints and clear commercial incentives to move faster.
Before selecting a tool, audit your current state honestly. What’s your actual no-show rate? Calculate it by month for the last quarter. How many calls go unanswered weekly? Time-track your reception team for one week—how much time is purely transactional versus relational?
Baseline metrics tell you where you’ll see gains. If your no-show rate is already 2%, AI won’t help much there. But if you’re at 18% no-shows and twenty unanswered calls weekly, the ROI case is compelling.
AI scheduling is not the future. It’s the current standard for competitive UK healthcare practices. Your patients already encounter AI booking in restaurants, hair salons, and dental practices. They expect it. Question isn’t whether to adopt this technology, but which vendor to trust with your patient relationships and when to start implementation.
Practices that integrate this effectively will operate more efficiently, grow faster, and deliver better patient experiences. Ones that don’t will increasingly struggle to compete as patient expectations shift toward instant, always-on access. That might sound alarmist, but look at the trajectory—evening and weekend booking is already table stakes. 24/7 AI assistance is simply the next logical step.
Start with your pain points. Fix those first. Expand capability as you build confidence. And remember: technology augments your team’s capabilities; it doesn’t replace human judgment and care that keep patients coming back.